.png) 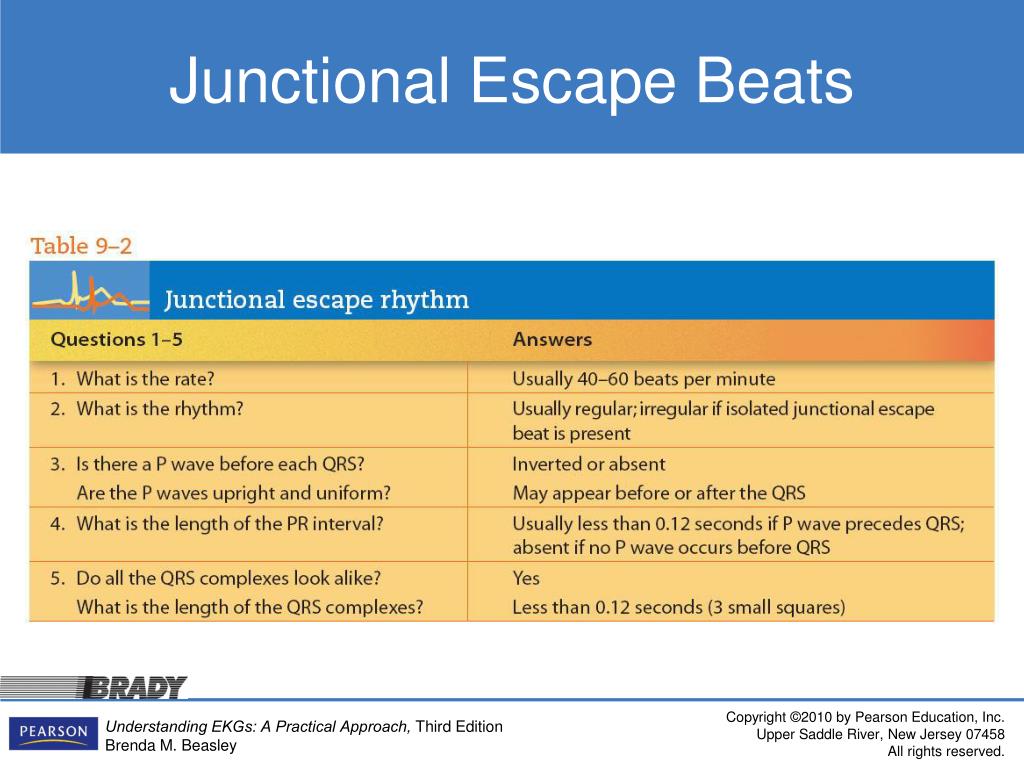
This document summarizes current developments in the field, with focus on new advances since the last ESC guidelines, and provides general recommendations for the management of SVT patients based on the principles of evidence-based medicine. To address this topic, a Task Force was convened by the European Heart Rhythm Association (EHRA) with representation from the Heart Rhythm Society (HRS), Asia-Pacific Heart Rhythm Society (APHRS), and Sociedad Latinoamericana de Estimulación Cardiaca y Electrofisiologia (SOLAECE), with the remit to comprehensively review the published evidence available, and to publish a joint consensus document on the management of SVT patients, with up-to-date consensus recommendations for clinical practice. In addition, several associated conditions where SVTs may co-exist need to be explained in more detail. There is a need to provide expert recommendations for professionals participating in the care of patients presenting with SVT. The European Society of Cardiology published management guidelines for supraventricular tachycardias (SVT) in 2003, 1 and corresponding US guidelines have also been published, the most recent being in 2015. Supraventricular arrhythmias are common, and patients are often symptomatic requiring management with drug therapies and electrophysiological procedures. Supraventricular tachycardia in pregnancy 498 Supraventricular tachycardia in adult congenital heart disease 496 The asymptomatic patient with ventricular pre-excitation 495 Wolff–Parkinson–White syndrome and atrioventricular reentrant tachycardias 492Ĭoncealed and other accessory pathways 494 Non-paroxysmal junctional tachycardia 492Ītrioventricular reentrant tachycardias 492 2008 Jul-Aug 36(4):691-8.Relationships with industry and other conflicts 467ĭifferential diagnosis of tachycardias 469Īcute management in the absence of an established diagnosis 475Īcute management of narrow QRS tachycardia 478Īcute management of wide QRS tachycardia 479Ītrioventricular junctional tachycardias 489Ītrioventricular nodal reentrant tachycardia 489 Anatomical aspects of the arterial blood supply to the sinoatrial and atrioventricular nodes of the human heart. Pejković B, Krajnc I, Anderhuber F, Kosutić D. Arterial blood supply of the atrioventricular node and main bundle. Van der Hauwaert LG, Stroobandt R, Verhaeghe L. Structure, function and clinical relevance of the cardiac conduction system, including the atrioventricular ring and outflow tract tissues. 1977 Jun 93(6):735-40.ĭobrzynski H, Anderson RH, Atkinson A, Borbas Z, D'Souza A, Fraser JF, Inada S, Logantha SJ, Monfredi O, Morris GM, Moorman AF, Nikolaidou T, Schneider H, Szuts V, Temple IP, Yanni J, Boyett MR. Correlations with electrocardiographic findings in 111 patients. Thery C, Gosselin B, Lekieffre J, Warembourg H. Normal sinus heart rate: sinus tachycardia and sinus bradycardia redefined. Junctional tachycardia: rate above 100 beats per minuteĬopyright © 2023, StatPearls Publishing LLC. Junction escape rhythm: rate 40 to 60 beats per minuteĪccelerated junctional rhythm: rate of 60 to 100 beats per minute Junctional bradycardia: rate below 40 beats per minute The terminology used to identify the type junctional rhythm depends on its rate and is as follows: This electrical activity then travels through the atria to the AV node from where it reaches the Bundle of His from where the electrical signals travel to the ventricles through the Purkinje fibers. Generally, in sinus rhythm, a heartbeat is originated at the SA node. 
A junctional rhythm is where the heartbeat originates from the AV node or His bundle, which lies within the tissue at the junction of the atria and the ventricle. The first septal perforator of the left anterior descending artery also supplies blood to the AV node. The blood supply to the AV node is from the AV nodal branch of the right coronary artery (90%) or the left circumflex artery (10%) depending on the right or left dominant blood supply to the heart. The sinoatrial nodal artery supplies blood to the sinoatrial node, it branches off the right coronary artery in 60% of cases, whereas in 40% of cases, it comes from the left circumflex coronary artery. This anatomic region is also commonly referred to as the triangle of Koch. It sits within an anatomic region bordered posteriorly by the coronary sinus ostium, superiorly by the tendon of Todaro, and anteriorly by the septal tricuspid valve annulus. The atrioventricular node (AV) is a subendocardial structure situated in the inferior-posterior right atrium. The sinoatrial node (SA) is the default pacemaker and is located subepicardially and is crescent in shape.
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
